8 Everyday Myths about IBD, Debunked
Learn More About Inflammatory Bowel Disease (IBD) from Digestive Healthcare Center
Inflammatory bowel disease (IBD) is a term used to describe conditions that create chronic inflammation in part or all of the digestive tract. Ulcerative colitis (UC) and Crohn’s disease are the most common conditions known under this umbrella term. Currently, in the U.S., about 780,000 people live with Crohn’s disease and 907,000 live with ulcerative colitis.
In honor of Crohn’s and Colitis Awareness Week, we’re helping to shed some light on these common diseases by dispelling some of the myths around them, some of which may even surprise long-term sufferers:
Myth #1: IBD and IBS are the same.
Fact: Though both may have overlapping symptoms—such as constipation, abdominal pain or urgent bowel movements— irritable bowel syndrome (IBS) is what’s known as a functional gastrointestinal disorder (FGID). FGIDs are the due to gastrointestinal (GI) tract dysfunction and are not the result of biochemical or structural (e.g., a tumor) abnormalities. IBD is classified as an actual disease, whereas IBS is not because of its status as a functional disorder. In addition, unlike IBD, IBS is a non-inflammatory condition.
Myth #2: Patients with IBD will end up having their colon surgically removed.
Fact: At the end of the day, treatments are based on each individual’s unique situation. A Crohn’s or UC diagnosis does not mean that surgery will be necessary. In actuality, many patients are able to manage their condition just fine with medications and other methods of treatment; surgery is typically a last resort to relieve symptoms.
Myth #3: Symptoms of Crohn’s and UC will disappear if patients cut gluten out of their diet.
Fact: Though everyone with Crohn’s or UC has different food triggers, removing gluten from one’s diet won’t have an impact on how the disease affects individuals. A gluten-free diet is only necessary for patients with Celiac disease. Patients should always speak with a specialist first before making any drastic changes to their diet.
Myth #4: Crohn’s and UC only affect the GI tract.
Fact: Many symptoms of IBD are, in fact, extra-intestinal. This means that they occur outside of the digestive tract. They can include joint pain, fatigue and even eye inflammation.
Myth #5: IBD is the result of stress.
Fact: This theory dates back to the 90s, and there is little evidence even now to suggest that IBD is due to stress, mental illness or traumatic life events.
Myth #6: Patients can suffer from Crohn’s and UC at the same time.
Fact: Despite their similarities, a patient cannot be medically diagnosed with both conditions. The confusion may come in if a patient is diagnosed with a disease called Crohn’s colitis, another IBD in which the pathology and biopsies indicate Crohn’s disease that is limited to a person’s large intestine. The name may imply to some that an individual has both diseases, which is not the case.
Myth #7: Remission of Crohn’s or UC is very rare and unlikely to happen.
Fact: Like treatments, results from managing each individual’s disease is unique. Patients should not take anecdotal evidence as gospel when it comes to their health. What is true for one person may not be true for another.
Myth #8: Patients diagnosed with IBD will never lead “normal” lives.
Fact: IBD can be a challenging issue to live with, but it does not necessarily hinder patients from living the lives they want to live. Patients should work closely with their medical professional(s) to effectively manage the disease and ensure an optimal quality of life.
For more information about Crohn’s or UC or to schedule an appointment with one of our specialists, contact us today.
Make an Appointment for Comprehensive Digestive Care in NJ
At Digestive Healthcare Center, we want each patient at our three offices in New Jersey to feel confident about their digestive health. We encourage you to contact us today to make an appointment with one of our expert gastroenterologists – don’t wait to start putting your digestive health first!
Recent Blogs
Learn more about all things digestive health and wellness by checking out our recent gastroenterology blogs.

Diverticular disease and diverticulitis are related digestive health conditions that affect the large intestine (colon). With diverticular disease, small, bulging pockets develop on the lining of the colon. When these pockets become inflamed or infected, the condition is called diverticulitis. They are very common – especially after age 40 – and rarely cause problems. At […]

Many Americans like to set New Year’s resolutions to make positive lifestyle changes such as improving their diet and going to the gym. However, March is also a great time for a healthy focus, especially as the long winter season comes to an end. National Nutrition Month, sponsored by the Academy of Nutrition and Dietetics, […]
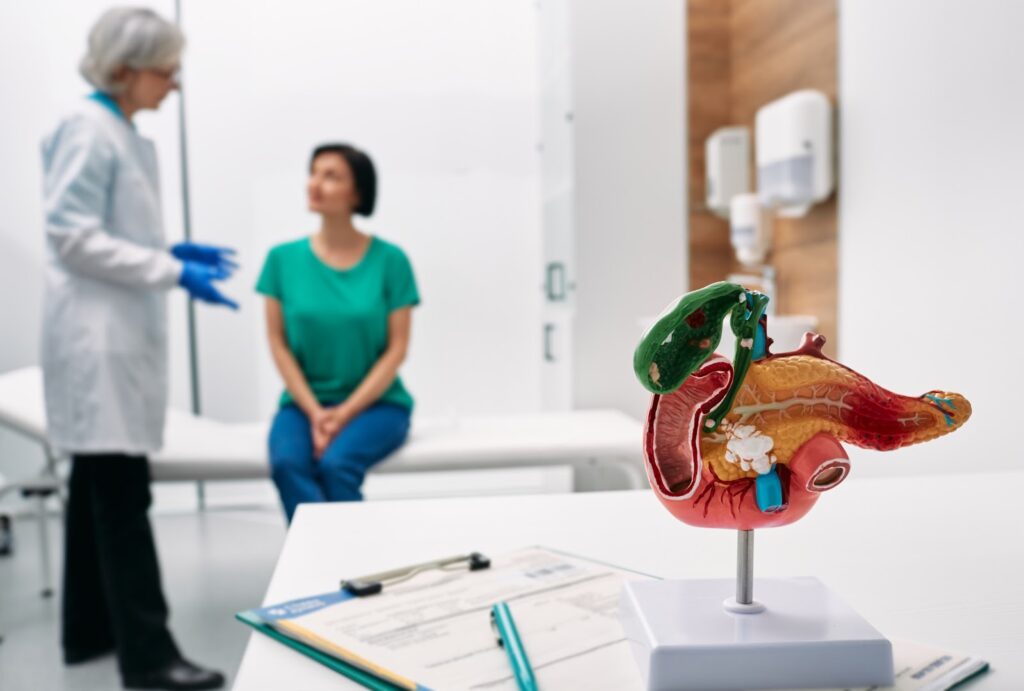
Gallstones form when bile stored in the gallbladder hardens. Your gallbladder is a small, pear-shaped organ on the right side of your abdomen, just beneath your liver. It holds a digestive fluid called bile that’s released into your small intestine. Gallstones are pebble-like pieces of concentrated bile material, typically made up of cholesterol or bilirubin […]